My apologies. It’s been a while since I’ve posted, and this has been intentional. I realized that I’ve just needed some time to unplug from this part of my life, but apparently, life is not as ready for me to be done with this journey just yet.
About a month ago, Ashley and I were sitting on the deck, drinking our coffee and watching the birds fly around the yard, in and out of their bird houses. However, something just didn’t look quite right – did she buy more bird houses?!
My worst nightmare had manifested itself again, but I wanted to give it a couple of days to see if was allergies or just a glitch with my eyes, so I let it go. If you’ve been following this blog, you know I could never be so lucky…
Back to the eye doctor I went. This is a new eye care center that I began going to last year and my doctor was not in the office on this particular day, so I saw someone new. She began to discuss the common causes of double vision, but I did most of the talking when I shared that this was not my first rodeo. Another possible explanation that is commonly seen is over-wearing of the contact lenses, which can lead eventually cause your eye to dry and contribute to double vision. “Let’s have a look!” she said. My left eye was extremely dry and the cornea had some scratching. But my right eye was perfect, and I wear contacts in both eyes for the same number of hours each day, so this really didn’t answer things for her.
We dove back into my medical history and the medications I am on. In 2019, at the young age of 35, I was diagnosed with glaucoma, a mystery in and of itself. To treat that, I am prescribed eye drops which I take twice per day.
“It’s possible the medication is causing the dry eye, but that’s an uncommon side effect of this medication, and it’s strange that it’s one eye only.”
“Let me take a look at something else” she said. Like a scene in a horror movie, my eyelids were then flipped up to get look at my lacrimal glands – these are what produce tears. The right eye was normal, but in the left eye, there was possible innervation damage to the lacrimal gland.
Neither of us actually said the words, but I know we were both thinking it – there was, and always will be, a possibility of a recurrence. It was suggested by the eye doctor that at my next MRI, I have imaging done of my orbits, to see the inner workings of my eyes. Another mystery to solve, and when I shared this news with my family, we all said “only me.”
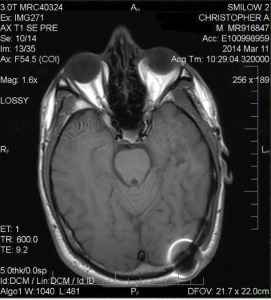
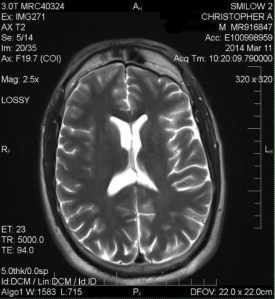
With many thanks to the wonderful team at the team at Yale, they scheduled me an appointment and got me in for scans last week. Double vision, double scans. Normally, I have a brain scan but this time, we added a scan of the orbits to see the inner workings of my eyes.
I think I spent more time and energy trying to keep my family calm, assuring them this was going to be fine and if there was anything there, I’d deal with it. I guess when you have dealt with this for so long, you become numb to it a little bit?
That following Tuesday, we arrived at Yale for a 7am MRI and while I lay on the cold slab of metal with the awful noises and banging from the machine, the only thing I could focus on was trying to breathe through the COVID face mask and the metal frame an inch above my face. Within a few hours, I received the long-awaited call and heard the news I knew was coming – you have a beautiful brain and the shunt is doing what it’s supposed to do. These words were such a relief to hear, but it led to the next question – why am I still seeing double then? Time will tell, as I am seeing a neuro-ophthalmologist this coming week.
None of this surprises me though – this has been the story of my life for the past fourteen years, and like everything I’ve been though, I’ll get through this and as the winds come, I will just keep adjusting the sails.
Recently, I was asked how this diagnosed changed me and I could tell by the look on the questioner’s face that my answer surprised her, but it was the honest truth. “It has been a hellish journey, but going through what I have has made me a better person and I am grateful for it.”
Like all brain tumor patients, brain cancer patients, and caregivers understand, this is, and will be, my cross to bear for the foreseeable future. No matter how positive the results, we face a lifetime of MRIs and testing, with the thought of the worst-case scenario lurking in our minds. I take solace in knowing that I have an amazing medical team looking out for me and the best family and friends any patient could ask for.
Fourteen years into this, life changed – perspectives changed. Anyone who has unfortunately undergone a life changing illness can likely attest to this, and while I would never wish this diagnosis upon anyone, this has been my blessing in disguise. No matter what, I have learned the importance of staying positive and hopeful. I now know that whatever obstacle comes my way next, I’ll keep smiling and doing the only thing I know how – maintaining a good outlook, being thankful for those around me and enjoying today.







 But alas, the frame had been affixed to my head. I don’t know what a vice feels like, but this sure as hell felt like what I would imagine.
But alas, the frame had been affixed to my head. I don’t know what a vice feels like, but this sure as hell felt like what I would imagine.

